IVF medications and protocols: EXPLAINED by a fertility doctor
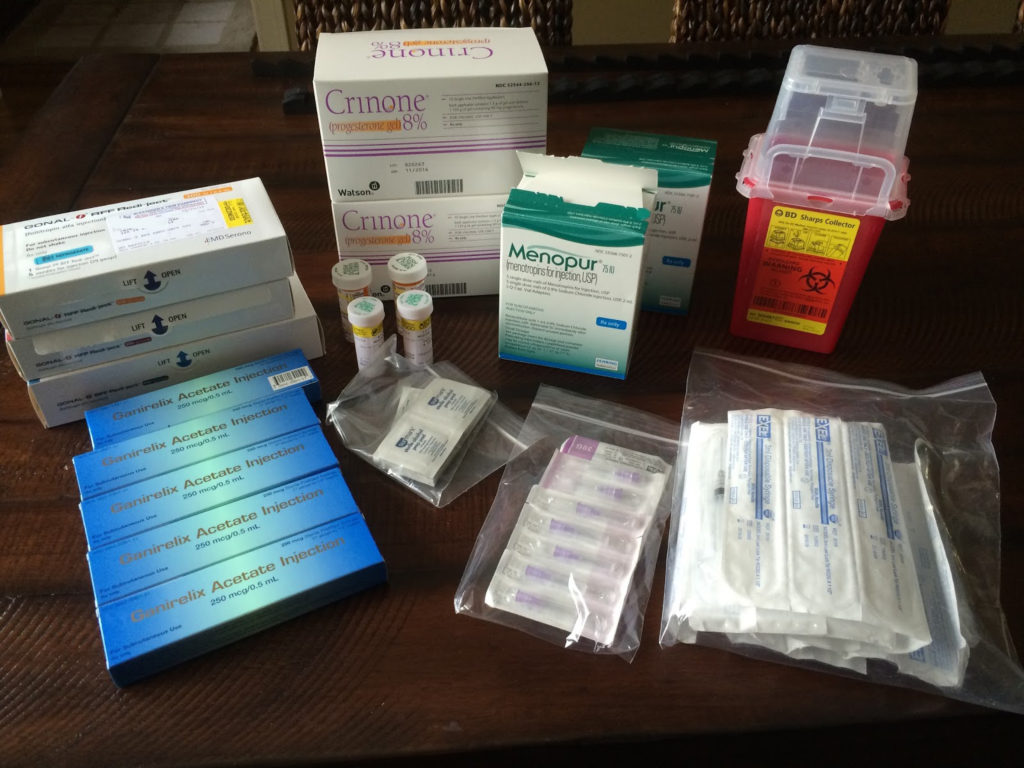
“Injections to ‘plump up’ the ovaries so we can extract the eggs.”
“Shots that jack up your hormones.”
These are just some of the ways I have heard patients describe the process of ovarian stimulation for egg retrieval. Whether egg freezing or doing IVF to freeze embryos or to get pregnant now, one of the most daunting aspect of the process is having to take injectable medications. For most patients, this is their first time ever injecting themselves with any medication. We decide on a protocol, a cocktail of different medications to be taken at specific points in the ~2 week process and then patients follow the instructions like a recipe out of a cookbook – as we make updates and adjustments along the way as they come in for check-in visits where we monitor the growth of the follicles (the bubbles of fluid that each hold a single egg) and their hormone levels, to gauge their response to treatment and to figure out the right timing for the egg retrieval.
But WHAT are these medications? How do protocols work? What are the pros/cons of certain types of ovarian stimulation protocols?
Buckle up – because I am going to break all of this down for you – but, first, it requires a clear understanding of how our ovaries work and the hormone signals:
Understanding Ovarian Biology
Every so often, there are a random, limited subset of the eggs which are recruited from the stockpile of eggs in the ovary – these become available to respond to hormonal stimulation. In a regular ovulation cycle, a hormone signal (called Follicle Stimulating Hormone (FSH)) from the pituitary is sent out at the beginning of the cycle (during menstruation) and it leads to the random selection of a follicle which then enlarges over the course of 1-2 weeks. Once the follicle is mature, it produces a certain amount of estrogen above a critical threshold which then signals to the pituitary gland telling it to release a second signal, called Luteinizing Hormone (LH) – this triggers the follicle to rupture and release a mature egg. The rest of the recruited eggs undergo breakdown and are wasted and can never be used again in a future cycle. When stimulating the ovaries in advance of egg retrieval, you are injecting these hormone signals (that naturally come from the brain to stimulate ovulation of a single egg) – but you are injecting these hormones at a higher level in an effort to select multiple follicles to grow and mature – not just the single one that would normally mature and ovulate naturally. The goal is to get every single recruited egg to grow and mature, because those recruited eggs will otherwise be discarded at the end of that cycle – at which time a new wave of recruited eggs will become available from the overall stockpile.
Step 1: Ovarian Stimulation
Medications like Gonal F and Follistim are synthetic versions of FSH. Menopur or HMG (human menopausal gonadotropin) are a combination of FSH and LH. This is why these medications are ALWAYS used as part of the protocol – they are the backbone of an IVF protocol and essential to the stimulation of multiple follicles. When we choose the dose of these medications we factor in the overall picture and patient diagnosis. For example, many women with PCOS may have high baseline levels of LH, relative to FSH, and we may give them relatively higher doses of FSH over menopur. In women who have really low levels of LH because their pituitary gland in their brain is sluggish (this commonly occurs in women with history of eating disorders or excessive exercise (ie. marathon runners), we may give higher doses of LH-containing menopur. Both the amounts and the ratio of FSH and LH matter when it comes to stimulating the ovaries effectively. Patients with low egg count often ask me if it is possible to increase the dose of medication to be more aggressive – it is important to know that beyond a certain level the receptors for FSH and LH become saturated – so increasing dosage above a certain point (I consider maximal dosing ~300IU FSH + 2-3 vials menopur) will not help and is not cost effective (meds are expensive!).
Step 2: Prevent Ovulation
We also need a strategy to prevent ovulation – because when follicles are mature they will eventually signal the brain to release LH and cause eggs to be ovulated – and we don’t want that! We want to collect the eggs with an egg retrieval procedure before they are released into the Fallopian tubes. We can prevent ovulation with 2 different types of medications:
- GnRH antagonist (Cetrotide, Ganirelix) – These meds oppose the actions of GnRH which usually stimulates the pituitary gland to release the LH hormone. The medication actually blocks receptors on the pituitary to prevent an LH surge. We normally start this when the lead follicle reaches a diameter of 14mm or estrogen levels approach levels of 600-700pg/ml. When starting this, we often bump the menopur dosing up by 1 vial to counteract some of the suppressive effect that the GnRH antagonist can have on LH levels.
- GnRH agonist (Lupron) – GnRH is a hormone that comes from the brain and has an interesting dichotomous impact on the pituitary gland’s production of the LH hormone. If given for a few days – it can lead to a stimulation or rise in FSH and LH levels from the pituitary, which stimulates the ovaries. If given over an extended period of time, it can actually ‘numb’ the pituitary and prevent the release of FSH/LH. This is the reason behind the confusing fact that lupron can be used to both prevent ovulation and suppress the ovaries as well as trigger pituitary stimulation of the ovaries including an LH surge. It all depends how it is given, and for how long. A one-time/short course will stimulate, whereas continued administration over time will suppress and prevent ovulation.
Step 3: The Trigger Shot
The final step in the protocol is the TRIGGER SHOT. This is the one that gets a lot of attention because it truly is time sensitive – to the hour! The idea is to mimic the LH signal sent from the brain to the ovaries which triggers final maturation of a follicle and ovulation of an egg. Knowing that it may take ~40 hours to actually cause the stimulated follicles to ovulate the eggs they contain, the egg retrieval is scheduled 36 hours post-trigger shot. The purpose of the trigger shot is to mature the eggs and ‘ripen’ the follicles so that the eggs are easy to detach from the wall of the follicle and collect during the egg retrieval. The trigger shot comes in a few different forms/combinations:
- Human chorionic gonadotropin (hCG) – This is the same hormone that an embryo produces when it implants – it is the pregnancy hormone! It has a VERY similar structure to the LH hormone, which is needed for ovulation. Therefore, taking hCG will bind the LH receptors on the ovary and cause ovulation within ~40 hours or so. HCG has a very long half-life, meaning it lingers in the circulation for very long – when taking hCG along it is typically given at relatively high doses (5000 to 10000 units) – this can lead to prolonged stimulation of the ovaries even after the egg retrieval and is a prime culprit behind ovarian hyperstimulation syndrome.
- Dual trigger shot (HCG + lupron) – In the early 2000s it was figured out that we could use lower/minimal doses (1000 units) of hCG and still adequately mature and retrieve eggs without compromising the overall outcome of the cycle. This is because we can also use lupron alongside smaller doses of hCG to also stimulate maturation of the eggs before retrieval. Using 40-80 units of lupron + low dose hCG is now commonplace and is one of the major reasons why hyperstimulation is less common as a complication of IVF. The lower dose of hCG leaves the circulation much more rapidly and leads to faster recovery post egg retrieval.
- Lupron-alone can be given in cases where the risk of hyper stimulation is so great (ie. young women with high response/PCOS) that even 1000 units of hCG would best be avoided. We can use lupron-only trigger, without any hCG, in patients who we know have functional pituitary glands which will release adequate amounts of LH in response to lupron (a GnRH agonist that works on the pituitary gland). Lupron-only triggers do not work on patients who are hypothalamic and do not release LH.
Now that we have identified all the players (types of medications and how they work), let’s talk about specific commonly used IVF protocols:
COMMON PROTOCOLS THAT USE LUPRON TO PREVENT OVULATION:
Lupron down regulation aka ‘the long protocol’
Here lupron is injected (usually 10 units a day) starting 1 week post ovulation OR randomly while on birth control pills to suppress the ovaries. If starting after ovulation, we expect menstruation within a week or so, at which time we typically drop the lupron to 5 units a day and start FSH/LH injections to stimulate the ovary. The lupron prevents ovulation throughout. The pretreatment lupron helps to suppress any lead break-away follicles from growing early on – so this protocol may help to synchronize the growth of follicles. It has also been proposed to help suppress LH-driven androgen production in the ovaries (hormones like testosterone) which can be problematic for the ovarian hormonal micro-environment in women with disorders like PCOS. Because the lupron is being used throughout the protocol, it cannot be effective as part of the trigger shot – so a downside of this protocol is that full dose hCG must be used for effective maturation and retrieval of eggs. Another potential downside is that the long duration of lupron use can be overly suppressive to the ovaries and increase the requirement of FSH/LH injections to achieve adequate stimulation of the ovaries in the lead up to the trigger shot.
Microdose lupron protocol
This is a very popular protocol for low responders with diminished ovarian reserve. Lupron is given in small ‘microdoses’ twice a day starting on day 2-3 of menstruation. Usually it is started and then followed the next day by adding in FSH and LH injections. Initially, the microdose lupron will cause a flare of activity in the pituitary gland and release more FSH and LH for the first two days, on top of the additional FSH and LH being injected – so there is almost a dual stimulation happening internally and externally. After a few days, the continued lupron twice daily will have a suppressive effect and prevent ovulation of the growing follicles. Again, because lupron was used throughout, it cannot be used as part of the trigger shot and full dose hCG is the only option for the trigger shot.
+/- Birth control pretreatment
Birth control pills can be used in the lead up to either cycle type – to hold the ovaries hormonally at day 3 of the cycle where all hormonal levels are baseline. We normally stop it and start injectable medications 4 days later. The microdose lupron can actually activate the old corpus luteum from ovulation in the prior cycle and lead to erratic rising progesterone levels early on in the cycle. For anyone planning a fresh embryo transfer 1 week after retrieval, it is important to use birth control pretreatment to prevent the premature rise of progesterone, which would mess up the window of implantation in the lining and reduce the chance of transfer success.
COMMON PROTOCOLS THAT USE GNRH ANTAGONIST (CETROTIDE/GANIRELIX) TO PREVENT OVULATION:
GnRH antagonist protocol
This protocol starts with FSH/LH injections and then we add in the GnRH antagonist drug (cetrotide/ganirelix) once the lead follicle approaches 14mm and/or estrogen levels approach 600-700pg/ml. Usually starting the GnRH antagonist calls for a slight bump up in the medication to counteract it’s suppressive effect on the ovarian LH receptors. I typically increase menopur by 1 vial, unless I am intentionally trying to pump the breaks a little on the response to stimulation.
+/- Priming the ovaries with either 10-21 days of birth control pills or a week of estrogen patch before starting the GnRH antagonist
This can be done to help prevent early recruitment and stimulation of lead follicles, to promote synchrony in the way the follicles grow and develop. I will typically use this approach in patients who have a prior history of a low yield of mature eggs (a low proportion (~less than 70%) of retrieved eggs were in the MII mature phase).
GnRH antagonist protocol + clomid/letrozole for 5 days at the start of injections
We can use medications like clomid or letrozole for the first 5 days of FSH and LH injections (they can also be staggered by a day or more) to produce a boost with release of FSH and LH from the pituitary, on top of the external stimulation from the shots containing FSH and LH.
GnRH antagonist protocols have a major safety advantage because they do not involve using lupron during the stimulation – therefore, lupron CAN be used as the trigger shot or as part of the dual trigger with a lower dose hCG injection. GnRH antagonist protocols have lower risk of OHSS because lower doses of hCG can be used – or even be omitted completely in cases where estrogen levels are very high and patients are at risk of hyperstimulation.
Things to keep in mind…
Something to realize when learning about these different protocols is that there is not a specific RIGHT or WRONG medications – it is sometimes trial and error – and there can be cycle to cycle variation within the same individual, regardless of the protocol used. As much as we would like it to be, choosing a protocol is not an exact science. There are certain rationales behind the choice of protocol, the dosage and ratio of FSH/LH, etc but you cannot predict a response to the medications until you go through the process.
I realize all of this information can be overwhelming – you don’t have to know the ins and outs of the medications you are taking and how it all works – that’s our job. But as a patient, I have found it helpful to fully understand the rationale behind the medicine to get a full picture and to feel more in control. It can also be helpful if you find yourself needing to do more than 1 cycle, to understand the tweaks and changes being made in your protocol – so that you can be an active participant in strategizing the road ahead with your doctor, rather than a passive observer (which can worsen the feeling of lost control). If you are reading this and preparing to undergo ovarian stimulation for the first time, here are some things to keep in mind that will make you feel less overwhelmed and maybe even more optimistic about your ability to withstand the process: no matter what the packaging says, all of the medications I have outlined here can be injected subcutaneously – meaning with a short, thin caliber needle that only needs to get through the skin and superficial layer of fat that lies under the skin. In contrast to intramuscular injection needs which are at least 2-3 inches long, subcutaneous injections are a walk in the park. Yes, the needles can lead to bruising where you inject – but these are usually non-painful and are always very temporary. And overall, the injections only last typically 8-12 days – it is surprisingly short-lived for all that you are accomplishing during that time.
I hope this thorough breakdown of the medications and protocols was helpful to your mental preparation and that these final thoughts help to put your mind at ease.
Please comment below and let me know if this was helpful and if you would like to get a similar breakdown of the various types of protocols we use for embryo transfer prep.


